Shingles is a viral infection that affects a nerve and the surrounding skin, caused by reactivation of varicella-zoster, the chickenpox virus. After varicella zoster causes chickenpox, mostly in childhood, it remains dormant in the body for life. The reactivation of the dormant virus is what causes shingles. Therefore, anybody who had chickenpox in their childhood has this virus hidden in their nerves.
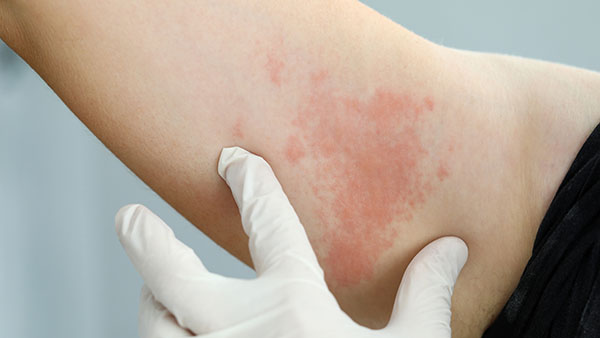 Shingles, also commonly known as herpes zoster, causes painful rashes on the skin and unusual pain on one side of a patient’s body. According to the Centers for Disease Control and Prevention, 1 of 3 people in the United States will develop shingles in their lifetime. Not everyone predisposed to the virus will develop shingles. As much as children can suffer from the symptoms of this viral infection, older people and those with weak immune systems are at an increased risk of developing shingles.
Shingles, also commonly known as herpes zoster, causes painful rashes on the skin and unusual pain on one side of a patient’s body. According to the Centers for Disease Control and Prevention, 1 of 3 people in the United States will develop shingles in their lifetime. Not everyone predisposed to the virus will develop shingles. As much as children can suffer from the symptoms of this viral infection, older people and those with weak immune systems are at an increased risk of developing shingles.
Other risk factors include emotional stress, injuries, or major surgery. Organ transplant surgeries require immune suppressors, and overly, the body is weakened and predisposed to activation of varicella-zoster.
Signs and Symptoms of Shingles
The appearance of shingles commonly starts with one-sided body pain and the formation of rashes on the torso, neck, and face, usually in small patches. The pain’s characteristic is as patches of burning sensation, which is followed up by the rashes. The rashes have a characteristic appearance as fluid-filled blisters and red patches with a stinging sensation. They may follow the nerve pattern they have affected and appear as a band on the body along the path of the affected nerve. The rash can spread as the infection progresses to other parts of the body. The extent of spread varies in people; it is not the same rate or magnitude. The fluid-filled blisters often break, dry, and form a crust. This process is painful and itchy until the dry crust completely heals.
 Although the onset of the rash and spread may take a few days to a few weeks, a person with a weakened immune system may have more severe symptoms that last longer. In certain rare cases, the virus can spread to organs such as the eyes and ears, causing infection and pain. Sometimes a severe infection can cause blindness, loss of hearing, and facial paralysis.
Although the onset of the rash and spread may take a few days to a few weeks, a person with a weakened immune system may have more severe symptoms that last longer. In certain rare cases, the virus can spread to organs such as the eyes and ears, causing infection and pain. Sometimes a severe infection can cause blindness, loss of hearing, and facial paralysis.
Shingles inside the mouth can lead to difficulty in eating and even loss of taste. In some instances, the rashes on the face may spread to the scalp and cause sensitivity of the hair follicles and hair loss. However, these are not the only appearances used to diagnose shingles. Other symptoms include:
- Fever and chills
- Headache
- Muscle weakness
- Lethargy
- Nausea
- Stinging or numbness of the skin
The average case of shingles can last up to 4 weeks. However, specific complications that develop could cause the effect to become permanent. For instance, a shingles complication called Post Herpetic Neuralgia (PHN) stays with the affected person long after the rashes have cleared. PHN is evident as pain in areas where the rashes were and can last from months to years.
Post Herpetic Neuralgia() can cause severe pain, leading to depression and anxiety, including weight loss. Although it is a rare complication, studies show that an average of 15% of people with shingles will end up developing PHN. The risks increase with age and low immunity.
Can Shingles be transmitted?
Shingles are not contagious; an infected person cannot transmit it to another. However, the active varicella virus in herpes zoster is transferable to a person who has never had chickenpox. The infection will then present as chickenpox.
Varicella spreads through contact with fluid from an infected person’s blisters. A patient with shingles is thus only contagious when the blisters have manifested. Before the blisters appear and after they dry out to crusts, there is no risk of passing the virus to another person anymore.
On can prevent transmission by covering the rash, washing hands frequently, and staying away from high-risk individuals (pregnant women, persons with low immunity and infants) or any person who has never had chickenpox or its vaccine. Recurrence is rare in the same person, but very possible.
Treatment and Medication
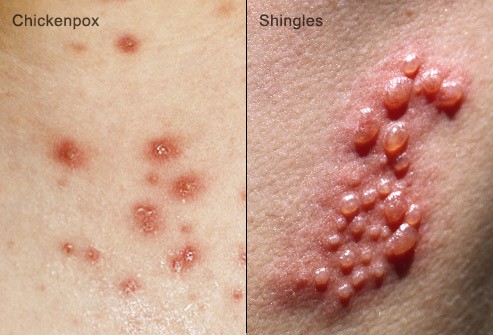
A shingles diagnosis is made first before beginning any form of treatment. Most diagnosis considers the history of pain, location of the problem, and the rash’s physical occurrence. However, some people may experience symptoms without a rash for a few days. Either way, seeking medical treatment is the best way to get help.
There is no cure for the virus that causes herpes zoster, but there are prescription drugs used to reduce the symptoms and prevent any severe complications. Most infections are manageable at home with a doctor’s advice and medicines. It is only severe cases and people with immunity issues that may require hospital admission.
Treatment includes administering antiviral drugs and using products such as shingles creams. The antiviral drugs are taken within 72 hours to minimize the spread of the rash and manage pain associated with shingles. Pain relief medication such can also help with pain management. The patient can purchase pain management drugs over the counter.
Other ways of relieving shingles symptoms include taking lukewarm oatmeal baths to reduce itching, using cold compressors for relief from the burning sensation, and soothing lotions for the rash. One can easily find shingles cream that are good for rapidly reducing pain, inflammation, and the itchiness associated with blisters.
For long-term preventive mechanisms, a shingles vaccine is an excellent choice for people who have never had chickenpox, those predisposed, and those who have had shingles before and want to avoid a second infection. However, a doctor’s advice is critical in understanding if one can take the vaccine and which type is safe. A vaccine can also help prevent PHN in older adults at risk of developing shingles.
Shingles can be incapacitating when severe pain is involved. With the risk of complications and severe infections, one should see a doctor as soon as symptoms appear. Self-care and keeping the immune system healthy can significantly help reduce the risk of activating the varicella virus.
